A dental implant is often the most reliable solution when restoring lost teeth. However, the long-term success of implants depends on many biological factors, one of the most critical being the oral microbiome. The oral microbiome is a delicate ecosystem of bacteria, fungi, and microorganisms that live within our mouths. When balanced, this ecosystem protects oral health, but when disrupted, it can lead to inflammation and complications such as implant failure. Understanding this connection can make a vital difference for patients considering a dental implant in Hereford, as it directly impacts healing, bone integration, and long-term function.
What Is the Oral Microbiome?
The oral microbiome is composed of millions of microorganisms that naturally inhabit the mouth. Many are beneficial, helping to prevent disease by maintaining balance. Others, however, are opportunistic and can cause harm when conditions allow them to flourish. Gum disease, tooth decay, and peri-implantitis often begin with shifts in microbiome balance.
For individuals seeking a dental implant Hereford, grasping this concept is essential. A balanced microbiome allows proper integration of the implant and reduces the risk of infection. Conversely, poor oral hygiene, smoking, or pre-existing conditions can disturb microbial balance, leading to long-term implant complications.
The Implant Process and Role of Microbiota
Dental implants work by fusing with the jawbone in a process known as osseointegration. For this to function well, the surrounding tissues must remain healthy. Harmful bacteria in the microbiome introduce inflammation, which delays healing and increases the risk of implant loss.
Implant placement involves minor surgery. Just as an emergency dentist in Hereford would stress during urgent care treatment, infection control is critical. From the moment the implant is placed, the wound site becomes a potential target for bacterial invasion. Good microbial balance minimises these risks, highlighting the importance of hygiene both before and after surgery.
Microbiome and Peri-Implant Diseases
One of the greatest threats to implant stability is peri-implant disease. There are two types:
- Peri-implant mucositis involves soft tissue inflammation.
- Peri-implantitis, where bone around the implant is also destroyed.
Both conditions are linked to imbalances in oral microbiota. Research shows that when pathogenic bacteria dominate, they trigger immune responses, causing tissue breakdown. Patients who regularly visit their dentist and maintain controlled oral hygiene are less likely to encounter these issues.
Key Benefits of a Healthy Oral Microbiome
- Promotes better implant healing during the early osseointegration phase.
- Reduces risk of post-operative infection and peri-implantitis.
- Supports long-term stability and success of implants.
Maintaining a Balanced Microbiome Before and After Implants
To improve the likelihood of dental implant success, it is important to keep the oral microbiome balanced throughout treatment. Just as one would consult an emergency dentist in Hereford if sudden oral pain struck, proactive measures before and after an implant procedure are crucial for prevention.
Regular dental visits should begin before implant surgery to rule out hidden gum infections or decay. Lifestyle adjustments such as quitting smoking and reducing sugar intake play a role in promoting beneficial bacterial growth. Even small changes in daily habits can reduce harmful biofilm and enhance recovery rates.
Patient Education and Preventive Focus
For patients, learning how to foster a healthy microbiome is just as important as understanding surgical details. Many implant failures are preventable with improved awareness of oral ecology. Brushing twice daily, using antibacterial mouth rinses when prescribed, and maintaining regular professional cleanings are proven measures. Support from a trusted dental professional ensures that microbial shifts are noticed and managed before they become serious.
Microbiome-Friendly Diet Considerations
Diet has a major influence on bacterial communities. Frequent intake of refined carbohydrates encourages harmful bacterial growth. Conversely, fibrous vegetables, lean proteins, and probiotic-containing foods such as yoghurt support beneficial bacteria. When balanced nutrition is combined with good oral care, the microbiome has better resilience to the stresses of implant surgery.
Comparing Microbiome in Natural Teeth vs Implants
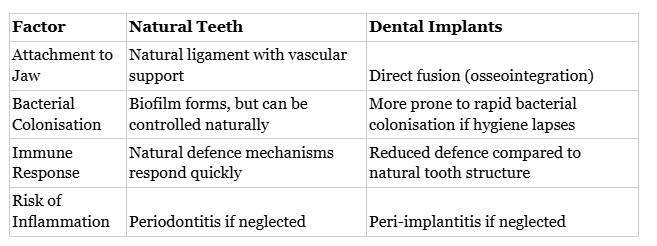
This table shows how implant success is closely tied to microbial control. Natural teeth offer more built-in defences, while implants require stricter long-term hygiene. This connection underscores the shared role of the patient and dentist in sustaining a healthy microbiome.
Oral Microbiome and Overall Health
It is important to remember that the oral cavity does not exist in isolation. Harmful microbial activity in the mouth can spread to other bodily systems through the bloodstream. Inflammation that begins near dental implants has been linked to systemic conditions, including cardiovascular disease and diabetes complications. Patients seeking a dental implant in Hereford should therefore understand that implant success is not only about tooth replacement but also about maintaining general well-being.
Professional Monitoring for Implant Longevity
Follow-up appointments are crucial, especially in the first year after implant placement. During these visits, dentists check for early signs of infection, microbiome imbalance, and stability of the new implant. An emergency dentist in Hereford might be called upon if sudden swelling or pain arises, but ideally, continuous preventive check-ups avoid such scenarios.
Clinics now sometimes use microbiome testing to assess risks before and after surgery. Saliva and plaque analysis can reveal bacterial patterns that guide tailored preventive care. In the near future, such tools may become routine in implant dentistry, offering even more precise strategies for success.

Steps Patients Can Take to Improve Implant Outcomes
- Regular dental check-ups before and after implant placement.
- Consistent oral hygiene with tailored professional guidance.
- Balanced diet low in processed sugars but rich in fibre and probiotics.
Video Link : https://rumble.com/v6qgpe6-restore-your-smile-with-advanced-dental-implants.html
Conclusion
The oral microbiome plays a decisive role in whether an implant thrives or fails. Patients who proactively balance their microbiota through hygiene, diet, and professional guidance experience higher success rates and improved quality of life. Whether consulting for routine care or visiting an emergency dentist in Hereford, understanding this link can transform outcomes. If you are considering a dental implant in Hereford and wish to explore personalised treatment plans, EDH is here to help you achieve lasting oral health.

